SYSTEMATIC REVIEW
Type 2 Diabetes Treatment and Drug Development Study
Da-Yong Lu1, *, Jin-Yu Che1, Nagendra Sastry Yarla2, Hong-Ying Wu1, Ting-Ren Lu1, Bin Xu3, Shu-Yun Wu3, Jian Ding3, Yi Lu4, Hong Zhu5
Article Information
Identifiers and Pagination:
Year: 2018Volume: 8
First Page: 22
Last Page: 33
Publisher Id: TODIAJ-8-22
DOI: 10.2174/1876524601808010022
Article History:
Received Date: 15/5/2018Revision Received Date: 5/7/2018
Acceptance Date: 16/7/2018
Electronic publication date: 31/08/2018
Collection year: 2018
open-access license: This is an open access article distributed under the terms of the Creative Commons Attribution 4.0 International Public License (CC-BY 4.0), a copy of which is available at: https://creativecommons.org/licenses/by/4.0/legalcode. This license permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The causality and etio-pathologic risks for patients with Type 2 Diabetes (T2DM) are important areas in modern medicine. Disease complications are largely unpredictable in patients with T2DM. In the future, we welcome therapeutics of both cutting-edge and traditional for anti-diabetic treatments and management with higher efficiency and less cost. Expanding medical knowledge, behavior/life-style notification in healthcare, modern genetic/bioinformatics diagnostic promotion, clinical developments (Traditional Chinese Medicine and personalized medicine) and new drug developments - including candidate drug targets should be implemented in the future. These efforts might be useful avenues for updating anti-diabetic therapeutics globally. This article aims at introducing this information for T2DM treatment boosts.
1. INTRODUCTION
The prevalence of Type 2 Diabetes (T2DM) is reaching a critical stage in developing and developed countries worldwide approximately 15% morbidity rates globally - including China, Indian, US and others due to lack of therapeutic options for disease cure in a great part of patients with T2DM [1-5]. For this reason, global medical expenses for anti-diabetic treatments are growing rapidly [1-5]. However, many key elements related to diabetes causality, pathogenesis and therapy are still waiting for the unveiling.
The quality of experimental or clinical diabetes study has been varied owing to the divergent patient’s physiological conditions, disease stage and therapeutic differences. Some agents might target on blood glucose level control and some others might be associated with insulin- or genetic-related pathways. As a tough medical challenge, new conditions may be met from the developments of multi-functional therapeutics. Different areas of top medical challenge to anti-diabetic managements are highlighted in the following sectors.
2. OVERALL LANDSCAPES
2.1. T2DM Causality and Etio-Pathogenesis
Developing T2DM might undergo a lengthy and complex course, even pathogenesis cascade processes, in susceptible human beings. Some of them are even partly family inheritable diseases, like obesity and hypertension. Yet the T2DM pathogenesis processes and cascade are often difficultly reversed. Onset stage can more easily slow down disease progression and reduce patient’s morbidity rates in general people. A reliable, long-lasting and multi-functional medical education of diabetes may arise the attention of wider populations, especially to old persons who are more susceptible to T2DM events. Given asymptomatic in early stages of T2DM, regular blood glucose level checkup in persons (>40 years old or in sedentary occupation) is introduced.
Apart from food consumption control, some other unfavorable factors, such as habitually heavy drunk, long-term depression, sleep problem, genetic mutations/variations, obesity or sleep apnea etc. [2-19]. can also be the culprits of T2DM causality and pathogenesis. Thus, regular medical checks including blood glucose levels and other metabolic syndrome should be monitored as early as possible.
2.2. The Type 2 Diabetes Causality List-up
The origin of T2DM is unclear and not fixed - including molecular pathways of insulin-insufficient as well as functional resistance. Following factors are suggested to be involved in this lengthy process of insulin-resistance and disease onset:
- Fetus nutritional insufficient
- Energy imbalance (overfeed or shortage of mobile activity)
- Bad habits (over drunk etc.)
- Heritage (genetic or epigenetics)
- Neural-appetite axis
- Sleep problem (apnea or insomnia)
- Lack of enough exercises (sedentary occupation)
- Mental depression
- Hormonal-related
- Other metabolic causality (obesity)
- Drug-related (liver function impairment)
Regarding this relevant etio-pathologic originality, different therapeutic intervention and anti-diabetic drugs are met with this metabolic abnormality.
The medical intervention for patients with diabetes at an early stage is a way of reducing further metabolic complication events and human mortality. To attain this goal, educational work to wider audience is noteworthy (Table 1).
| Population Categories | Information |
|---|---|
| Doctors in big hospital Doctors in rural or remote area Medical students in colleges |
New ideas and clinical paradigm establish Ways of type 2 diabetes diagnostics & treatments in rural area Interests in diabetes study, Basic knowledge of diabetes |
| Pharmacologists Pharmaceutical scientists |
Different modes of diabetes treatments and drug development Different types and forms of therapeutic drugs |
| Patients with T2DM General populations at high risks Normal people |
Understand the relationship between diagnostics and treatments Awareness of diabetes-induced complications Aware the seriousness of disease, regular blood check (>40 yrs) |
3. DRUG DEVELOPMENTS AND THERAPEUTIC VERIFICATION IN THE CLINIC
3.1. Patho-Therapeutic Processes
Deeper understanding into pathologic/pharmacologic processes as well as mechanisms of action of a number of anti-diabetic drug is noteworthy and indispensable. To develop targeted drugs (higher therapeutic-index), pathology-pharmacology association study (diabetic progress and complications), especially in the field of human heritable characters and genetic predisposition must be boosted [11, 12]. But it still needs a longer time to finish.
In the initial stage, doctors and pharmacologists focused on blood glucose control - interfering or sabotaging food intake and digestions with compounds similar to glucose. To promote new therapeutic ideas, the top culprit of T2DM should be diversities and widen - at least not solely dependent on glucose itself. Accordingly, we should not rely on one or two therapeutic pathways. Novel events should be noticed and identified from experimental and clinical study.
In the real pathogenesis scenario of T2DM, insulin-binding or -related metabolism dysfunction, such as loss functions of pancreas island ß-cells [17], liver metabolism problems [18], insulin resistance [19] and other heritable mutants and variations by unfavorable family lineages) are noticed (Table 2). According to this concept, many in vitro glucose-related studies are especially difficult to realize. Due to this limitation, anti-diabetic therapeutic study is widely debated. To overcome this obstacle, new experimental model selection (animal) or clinical developments must be established. Current pathogenesis and mechanisms of anti-DM drugs are generally outlined in Table 2 according to pharmacological categories [11, 12].
Generally speaking, chemo-therapeutic drugs for T2DM are not without toxicity. Though many chemotherapeutic drugs for T2DM are not very toxic comparing with other drug categories, their therapeutic responses need a relatively long term to exhibit and incurable. Prescribing optimal drug doses or schedules in specific diabetes conditions in individual patients has to be renewed and wider application. Long-term adjustments for drug dosing and schedule require interaction and cooperation between doctors and patients (Table 2 and Fig. 1). As a result, large-scale pharmacologic or clinical study is indispensable and long awaited.
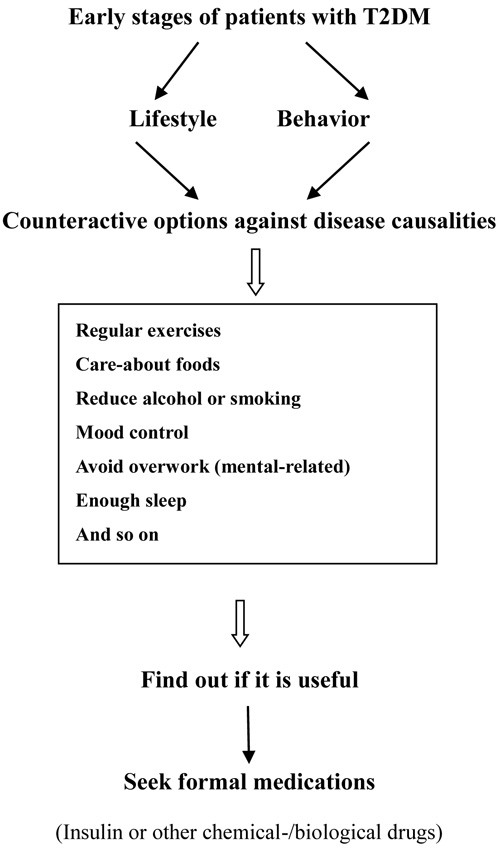 |
Fig. (1). Preventive and treatment measures for patients with T2DM. |
| Targets | Pathways and Symptoms | Personal Opinions |
| Glucose | Decrease glucose concentrations in animal and human by glucose metabolism interference Substitute or compete food glucose intake with other mono carbohydrates or glucose-derivatives |
Controversy Controversy |
| Insulin | Human insulin and its derivatives Modulators of pancreatic island ß-cell Muscle content and insulin-receptor Pharmaceutical innovations (oral forms of insulin) |
First line therapy Potential Important Future trends |
| Disease complications | Cardiovascular complications Nephropathy Obesity Chronic leg infection etc. |
Potential and need to be improved |
| Hepatic functions | Ameliorate of damaged cells and metabolism | Future trend |
| Genetic changes | Gene therapy or other biomedical therapies | Promising |
| Leg ischemic | Surgery | Not satisfactory |
| Life styles | Educations Regular exercise Lifestyle and behavior changes |
Adherence Persistence |
4. OVERVIEW OF CLINICAL STUDIES
4.1. Personalized Diabetes Therapy (PDT)
It is possible that the clinical symptoms, stages and event of blood glucose escalation may vary among different people in the clinic, especially in the aspect of human genome. As a result, T2DM treatments for each patient should not be uniform. PDT based on genomic alterations may be a futuristic medical hot-spot that will enable doctors to provide optimal therapeutics for individual patients with T2DM [19-23]. Nonetheless, PDT should not be restricted to pharmacogenetics (PG) technology alone as it is now solely reliant in the clinic globally [19-25]. At this stage of technical capability, PG study mainly focuses on drug concentration in human blood by detecting Single Nucleotide Polymorphisms (SNPs) of human metabolic enzymes (approximately 300 metabolic molecules in normal human body), modern chromatography and capillary electrophoresis. Despite a lot of PG study and report for diabetic therapy, it is not applied as diagnostic routines in general hospitals worldwide. Like PG for cancer treatment [23], approaches outside of the scope of the current diagnostic/therapeutic system might be invented in the future.
4.2. Bioinformatics and Metabolomics Techniques in the Clinic
Bioinformatics/metabolomics techniques for diabetic pathology and treatments are more straightforward compared with genetic information variations and explanations (Fig. 2). Fig. (2) depicts an outlook of different possibilities of PDT under investigations. This type of PDT may be utilized in future anti-diabetic treatments and have a great potentiality and biomedical significance other than PG.
5. PHARMACEUTICAL AND PHARMACOLOGIC INVESTIGATION
5.1. Higher Therapeutic-index Drug Developments
Since only small spectra of drugs can play a decisive role against T2DM, anti-diabetic drugs may be given life-long. An ultimate goal of drug developer and pharmaceutical company is to produce a reliable, safe and low toxic drugs. Likely, it is one of the major avenues in the fields of T2DM therapeutic studies and clinical drug applications [25-29].
Many synthetic drugs are commonly cheaper yet low therapeutic-index for human disease treatments. As the safest and first-line anti-hyperglycemia therapeutics, insulin and insulin-derivatives can be used for both type I and type II Diabetes mellitus therapeutics according to different lines of clinical situations [26]. Yet it is very difficult to adjust insulin dosage in these patients. It also has some drawbacks - injection syringes after food intakes. Besides, it is not always good news for possible low blood glucose levels (3.5-3.8 mmol/L) due to insulin or drug overdosing (a life-threatening event).
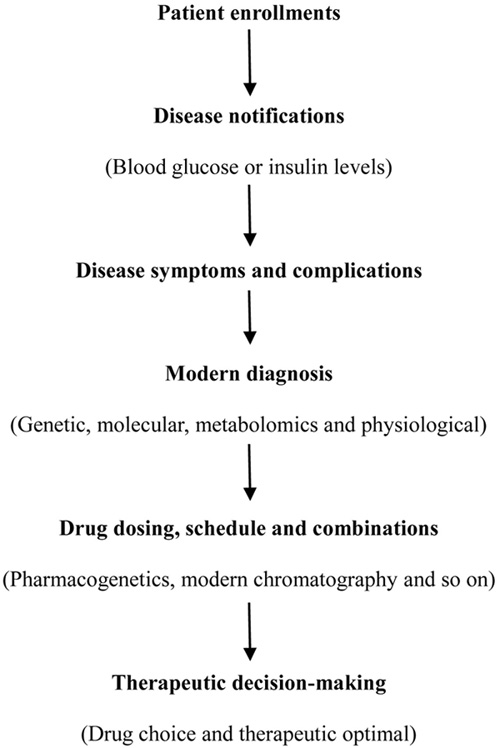 |
Fig. (2). Proposed diagram of personalized Diabetes mellitus therapy. |
5.2. New Drug Pharmaceutical Designs
Currently, oral intake of drugs is an environmental-friendly option for general patients. In the future, large-pool of small-molecular chemical pipelines by a computing system may add promising drug categories for T2DM [24]. If breakthrough achievement, new generations of highly effective, pharmaceutical-friendly chemical agents might be developed for oral insulin-like therapeutics for patients with T2DM [28-31].
6. NATURAL CHEMOTHERAPEUTIC DRUGS, HERBS AND MEDICINES
6.1. Traditional Chinese Medicine (TCM)
TCM has a long history and reports to notice many symptoms of diabetes. Certain numbers of herbs and recipes have been described in TCM books and legends to counteract with these unfavorable symptoms and diseases. As modern Chinese pharmacologist and doctors, we offer a brief introduction to this matter.
From the views of TCM, type 2 diabetes is likely as symptoms categories of blockage of key factors for physiological circulations or pathways; include (Tan-Shi-Ti-Zheng 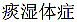 damp-phlegm syndrome); (Shi-Re-Ti-Zheng,
damp-phlegm syndrome); (Shi-Re-Ti-Zheng, 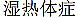 damp-heat syndrome) or (Xue-Yu-Ti-Zheng,
damp-heat syndrome) or (Xue-Yu-Ti-Zheng, 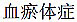 - blood/qi circulation stasis and syndromes). Doctors may prescribe patients with this herbal mixture against the abnormality of physiological circulations or pathways.
- blood/qi circulation stasis and syndromes). Doctors may prescribe patients with this herbal mixture against the abnormality of physiological circulations or pathways.
Many natural plants or organisms (>500 species) are proposed to show therapeutic against type 2 diabetes globally. They are a commonly crude plant, insect or animal products. Crude plants include leaf of Cyclocarya paluris , mulberry leaf
, mulberry leaf 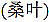 and root of remembranous milk vetch
and root of remembranous milk vetch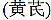 , milk thistle
, milk thistle and many others.
and many others.
Good therapeutic drugs need to not only reduce blood glucose levels but also act on wholesome physiological conditions in human beings. Natural chemotherapeutic drugs or other ancient therapeutic options are more suitable to meet with this modern challenge [32, 33].
6.2. Supportive Agents
Besides herbal medicine, some examples of insect or food products are also widely recognized to control the symptoms of T2DM [34-36].
Propolis is bee extract of waxy-like components extracted from crude honey. It was licensed as healthy-promoting agents yet practiced as hyperglycemia control for patients with T2DM [34, 35].
In Japan, some fermented soybeans (Natto) are also famous for T2DM-induced metabolic complication therapeutics. These fermented soybeans (Natto) can smooth human blood vessels (diabetes-induced cardiovascular complications), break phlegm-damp syndrome, blood/Qi stasis and many others [36]. Similar products will be developed against T2DM in new pathways.
6.3. Biotherapy
Since diabetes is a metabolic disease from endocrine abnormality, human biomolecules (such as insulin, micro-RNA, genomic modified bio-agents and so on) might be unique options for the disease control. However, most of the biomolecules are short-lived. Thus, pharmaceutical processes to add organic ligands/chains to bio-molecules (new delivery systems) are common routes for pharmaceutical purposes [26]. These processes are commonly less toxic and long-lasting.
7. DRUG COMBINATION
Drug combinations have been a paradigm for the management of many refractory diseases, such as cancer metastasis [37-40], HIV/AIDS treatments [41-43] etc. Since diabetes, especially T2DM exhibits wider spectra of symptoms, complications and genetic alterations in individual patients that need drug combination to overcome. A lot of questions should be answered - including how to choose drug combination before clinical applications. In our past arguments, optimal drug combination could be greatly improved from the therapeutic study of each possibility [37, 38]. It is however still at infancy stage currently.
Currently, even though a number of drug combinations have been utilized in clinical anti-diabetic treatments, theoretical medical studies are lag behind. Now clinical drug combinations are generally learned from doctors’ empirical and instinct rather than modern diagnostic supporting. In the future, clinical drug combination should be verified in each possibility [39, 40]. This type of medical work must be introduced from other medical disciplines, like cancer treatments [41, 42] and HIV/AIDS [41-43]. Let’s pay more attention to this matter in the future.
8. LIFESTYLE ADJUSTMENTS
Lifestyle adjustments mainly represent physical exercises as well as food intake precaution. In this practice, exercise duration, intensity and regularity must be noticed. Lifestyle adjustments and drug therapy is a famous clinical paradigm worldwide.
9. DISEASE CO-MORBIDITY AND COMPLICATIONS
9.1. Clinical Conditions
Diabetes co-morbidity and complications are a multitude. More seriously, most of them are even life-threatening if we do not prepare for them. Large parts of disease complications are difficult to be a reversal after their advents. As a result, diabetic-induced complication treatment study must be strengthened in the futures. This strategy is indispensable yet only a few of them, such as Propolis or α-thioctic acids are entered into markets. In co-morbidity disease, metabolic changes and chronic infections are widely presented [44-52] (Table 3).
| Complication Categories | Co-morbidity |
|---|---|
| Metabolic | Cardiovascular (atherosclerosis, hypertension, stroke) Obesity Muscle malformations Osteoporosis Keton-urea |
| Eye complications | Visual damage and blur Cataract Fundus hemorrhages and vessel leakage |
| Infections | Skin Legs |
| Kidney failure | Nephropathy |
| Cancer | Colon cancer and so on |
| Brain damage | Cognitive impairments Tiresome feeling and insomnia Lack mental concentrations Mental depression |
9.2. Co-Morbidity and Therapy
Many diabetic-induced complications are associated with blood AGE (advanced glycation end products) escalated by glucose metabolisms in the patient body. To those T2DM patients with higher blood AGE, propolis, α-thioctic acids and so on can reduce AGE and disease complications for a long-term. Correspondingly, drug combinations are unavoidable.
10. FUTURE PERSPECTIVES
10.1. Key Medical Challenge
Presently, anti-diabetic therapeutics has been standardized (Table 4). Expensive or cheap drugs are not parallel between their efficacy and costs. Since a growing number of patients are suffering from T2DM and co-morbidity worldwide. Anti-diabetic therapy studies need to boost. Persistent efforts and novel ideas are driving force for relevant drug developments (Fig. 3). Table 5 categorizes major avenues for achieving effective therapeutics in the future.
| Drug and Therapy | Mechanisms of Action | Adverse Events |
|---|---|---|
| Insulin and its derivatives | Glucose metabolisms | Not significance |
| Sulphonylurea | Stimulate insulin secretions | Gastrointestinal (20-30%) Infections (20%) |
| Biguanide (Metforrnin) | Decrease amount of sugar productions by liver | Metabolisms |
| Acarbose Voglibose |
α-glucosidase inhibitors | Gastrointestinal (20-30%) |
| Pioglitazone | Receptor agonists | Heart failure (1-5%) Bladder carcinoma (1-2%) |
| Exercise | Mimics insulin actions | Not significance |
| Curcumin Resveratol |
Plant chemicals Wider biochemical pathways |
Low |
| Other melbine | Variable | Variability |
| α-thioctic acids (Lipoic acid) | Disease complications | Not obvious |
| New anti-diabetic drugs | SGLT-2 inhibition DPP4 antagonists |
Under investigations |
| High therapeutic-indexed drug developments Educate wider ranges of audience to know the basic diabetic information Deeper understanding the relationship between causality, pathogenesis and therapeutics Genetic, epigenetic or molecular study of all relevant disciplines. Learn from minority medicines - such as Traditional Chinese Medicine, Indian/Pakistan medicine, middle-east medicine and so on Personalized diabetes therapy Establish therapeutics against disease complications Drug combination study, both experimentally and clinically Strengthen the scientific investigations of biotherapeutic activity and pharmaceutical delivery systems Budget control in drug developments and cost-effective in clinical trials Find out some small-molecular synthetic or natural chemicals with insulin-like functions and receptors-binding activities Find out some genetic targets from human genomes Genome Wide Association Study (GWAS) between patients and normal people Invite mathematic-/physics-majored scholars in anti-diabetic study Pharmaceutical innovation of insulin treatments from needle to oral Global cooperation in foundation areas |
 |
Fig. (3). Overall drug development and clinical utilities. |
10.2. Therapeutic Limitations
Co-morbidity and complications is a top priority and of great medical/pharmacology significance [52-55]. Since the relationship between hyperglycemia and co-morbidity symptoms has not been fully established, it is difficult to battle both sides of etio-pathologic processes.
Since too many pathologic molecules, components, steps and pathways can be changed in patients with T2DM, more patents for diabetic treatments are welcome across the world [53-55]. Continuing financial supports for anti-diabetic study are indispensable, especially genomic study and mathematical or computational study [56-58].
CONCLUSION
Treatment of patients with T2DM is still a medical challenge for a diversity of disease originality, pathogenesis and therapeutics of cutting-edge (new generations of biotherapies) and traditional (herbal or insulin-related). Certainly, optimal therapeutic strategies by traditional and new drugs in the clinic are a trendy movement. The healthy dissemination of diabetic knowledge to a wider audience is an excellent avenue in diabetic epidemic control. In the future, medical perspectives and novel drug developments will be implemented for changing the landscape of anti-diabetic therapeutic study.
CONSENT FOR PUBLICATION
Not applicable.
CONFLICT OF INTERESTS
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
This work was funded by Shanghai Science and Technology Foundation of High Educations 97A49.




